When summer rolls around, many Canadians are used to dealing with pests – be it mosquitoes out in the yard or ticks when walking in the forest. But in a warming world, these pests are likely to be more than just a nuisance. Climate-driven infectious diseases carried by insects such as mosquitoes and ticks are increasing in parts of Canada, and are expected to continue increasing as the climate changes.
Insects aren't the only cause for concern. Infectious diseases can also be carried in food and water, and are expected to be affected by climate change as well. Changes in temperature and precipitation, and extreme events such as floods and droughts can have significant impact on the range and spread of infectious diseases.
The ways that infectious diseases may be influenced by climate change are complex and the research is constantly improving. Health researchers have identified some vector-, food-, and water-borne diseases which are likely to be of significant concern for the health of Canadians in the future. This work helps us be aware of how infectious diseases are changing so we can better protect our health.
How does climate change impact infectious disease?
Infectious diseases are illnesses caused by tiny organisms such as viruses, bacteria, fungi, or parasites. While some of these organisms are harmless or even helpful to us, the ones that cause illness are called pathogens. [1] More than half of human diseases from pathogens have worsened due to climate change. [2] The changing climate is expanding the areas where vectors and pathogens can thrive.
We can be exposed to harmful pathogens through everyday actions, such as:
- Breathing in contaminated air
- Touching contaminated surfaces
- Eating or drinking infected food or water
- Being in close contact with sick people or animals
Watch the Animation: The Risks Are Real - Infectious Diseases in a Changing Climate
The health of every life form on earth is affected by the changing climate, from tiny microbes, to the vast boreal forest. Some impacts of climate change are visible, like more frequent and severe forest fires, where the smoke is harmful to our health. However, there are other things that can make us sick that we cannot see.
Climate change is causing temperatures to rise, and as regions get warmer, they become more suitable for organisms that could not live there before. This changes where and how often humans come into contact with these organisms, and can increase the possibility of becoming infected. In addition to shifting ranges, warmer temperatures also speed up the reproduction of vectors and pathogens. For instance, mosquitoes breed and mature faster in warmer conditions, allowing them to spread diseases more quickly. [3]
Climate hazards like flooding further change the distribution of vectors by creating ideal breeding grounds. Standing water from increased rainfall can increase mosquito populations, leading to more contact between humans and the disease-carrying vector. These environmental changes driven by climate change heighten the risk of illness by increasing both the number of pathogens and the chances of human exposure.
Categories of Infectious Diseases
Infectious diseases are categorized by how they are transmitted. Below are the different types of infectious diseases, and some of the ways that climate change is affecting them in Canada.
Zoonotic and Vector-Borne Diseases:
Zoonotic and vector-borne diseases are caused by pathogens that are transmitted directly by animals or insects when they come into contact with people.
Some diseases need a vector to pass from infected animal to human. Usually this happens through the bite of an insect vector, such as a mosquito or tick. [4]
These diseases can be transmitted by:
- Direct contact or close proximity to animals
- Airborne, waterborne, or foodborne transfers
- Vectors
Climate change impacts zoonotic and vector-borne diseases by affecting the populations of animals and insects, where they can be found, and how often humans come into contact with them.
For example, milder winters and longer, hotter summers can improve rates of survival, growth, and reproduction for some vectors like ticks, while also making new areas suitable for them to thrive. Read about how climate change affects black-legged ticks and lyme disease in the Lyme disease and climate change article. [5]
We could also start seeing new disease-carrying species of insects in Canada as the climate warms. For example, the Aedes Aegypti mosquito that can carry diseases such as Dengue, Chikungunya, Zika, and Yellow fever viruses is expanding its range northward through the US as the climate changes. There is concern this mosquito, and the diseases it carries, may make its way to Canada. [6] Read about mosquitos and diseases found in Canada in the Mosquito-borne diseases and climate change article.
Food-borne Illnesses:
Food-borne illnesses occur when the food we consume is contaminated with harmful pathogens. Eating raw animal products, fruits and vegetables cross-contaminated by animal products, or food washed with contaminated water are examples of ways we can become exposed to foodborne illnesses. [7] A warming climate can allow pathogens to survive longer and in new locations, increasing the likelihood that the food we eat has been exposed to harmful bacteria like salmonella, listeria, E. coli, or campylobacter. [8][9]
Factors such as air and water temperature, as well as precipitation, influence the growth, abundance, and survival of pathogens. These pathogens can find their way into crops, livestock, the environment, and eventually onto our plates. How we handle and cook our food also plays a role in the spread of these diseases.
Certain foods, like undercooked meat, shellfish, and raw vegetables, are more likely to cause food-borne illnesses. Research suggests that recalls for leafy greens and seafood are on the rise. [10]
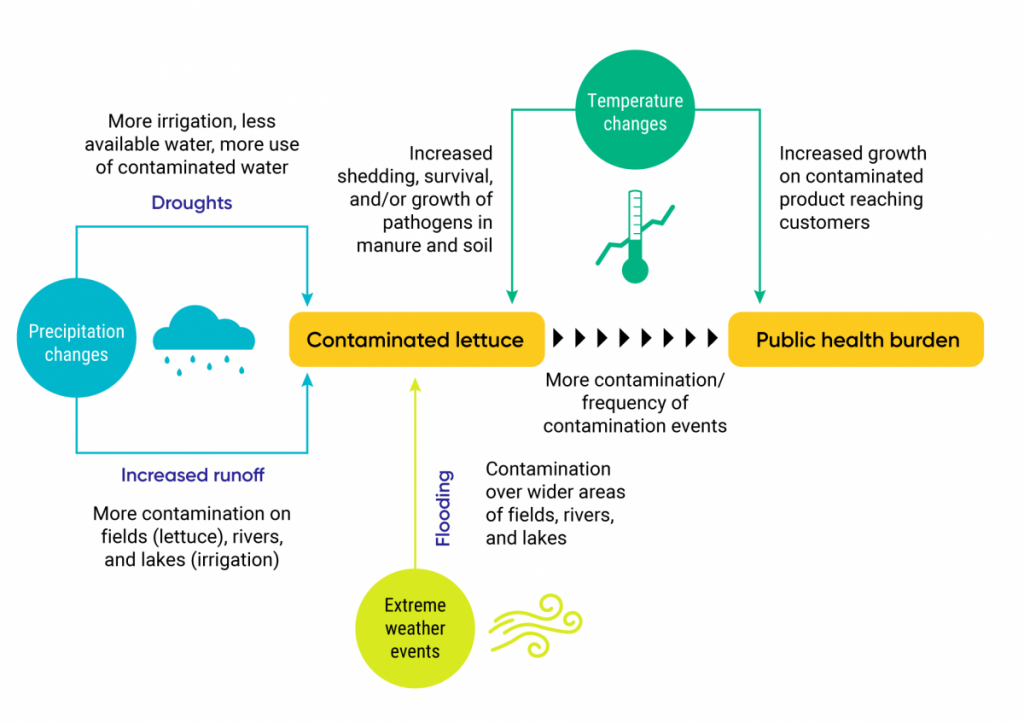
For example, leafy greens such as lettuce can be impacted by changes in precipitation that increase instances of contamination, extreme weather events that spread contaminants, as well as temperature changes that promote pathogen survival rates. [11] By understanding how we are exposed to pathogens and adopting better food-handling practices, we can reduce the risk of becoming sick.
Water-borne Illnesses
Sometimes pathogens can find their way into our water. When we get sick from consuming contaminated water, we call this a water-borne illness. Climate change is increasing the risk of waterborne illnesses by disrupting natural water systems. Canadian lakes are warming due to longer, hotter summers. Warmer water promotes the growth of harmful algal blooms, especially in regions like the Great Lakes and the Prairies, which can produce toxins harmful to humans and animals. [12] These risks are amplified in smaller or rural communities where water treatment systems may be less robust.
More frequent heavy rainfall events can flood wastewater and stormwater infrastructure, causing untreated or partially treated sewage to enter rivers, lakes, and other freshwater sources. This raises the risk of contamination with pathogens like E. coli, Giardia, and Cryptosporidium, which can lead to gastrointestinal illnesses. [13] As climate-related weather extremes become more common, the potential for waterborne disease outbreaks in Canada increases.
Our risk of waterborne illnesses is connected to the food we eat, the water we drink, and the ways we interact with water. Read more in the waterborne disease and climate change article.
Read More: The Environment, Human and Animal Health are Closely Connected
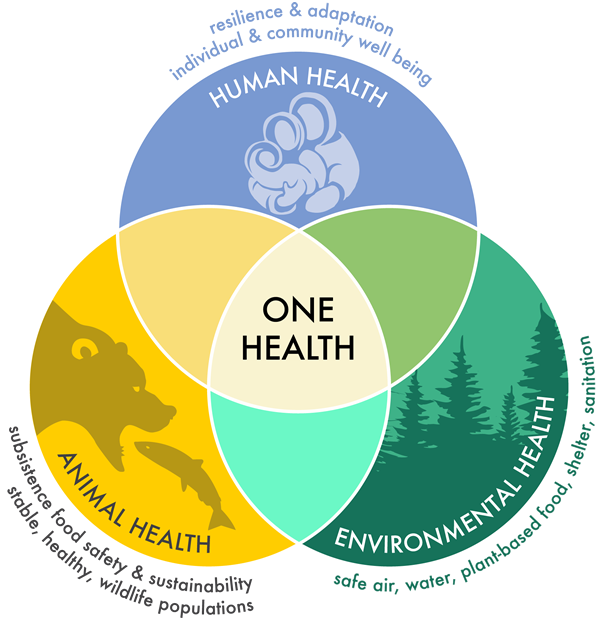
The idea of One Health explains human health, animal health, and the health of our environment are deeply connected. Diseases can pass between animals and people, especially as human populations grow and move into new areas. When forests are cleared, land is used for farming, or natural habitats are disturbed, animals and people come into closer contact, increasing the chance of new diseases emerging. Climate change adds to this risk by changing where animals and insects live, increasing extreme weather events, and disrupting natural ecosystems. [14]

Public health focuses on protecting and improving the health of people and communities. This includes preventing disease, promoting healthy lifestyles, ensuring clean water and air, and responding to health emergencies. [16] Climate change affects public health by increasing heat related illnesses, worsening air quality, threatening food and water supplies, and allowing certain diseases to spread more easily.
Planetary health looks at the bigger picture. It recognizes that human health depends on a healthy planet and “focuses on ways that human-caused disruptions to the Earth system affect human health.” Issues such as climate change, pollution, and loss of biodiversity can damage the natural systems we rely on for food, water, and clean air. [17]
Together, these concepts highlight the same message. Caring for our environment is essential to protecting our health now and in the future.
Strategies to reduce risk of infections
We can change our exposure to risks by changing our behaviour. Increasing awareness is the first step. Being more aware of the pathogens that exist in our environment and the ways we come into contact with them, and adjusting our behaviour accordingly will help us reduce our risks.
Outdoor Safety:
- Be aware of local environmental risks, such as posted swimming advisories, when planning outdoor activities like visiting the beach, and adjust plans accordingly.
- Protect yourself from insect bites by wearing long sleeves and tucking pants into socks. Use insect repellents and check for ticks after being outside. [18][19] If you notice signs of an infected bug bite, such as a bullseye rash, seek medical attention.
- After swimming in outdoor bodies of water, wash with soap and clean water to remove any potential pathogens you may have come into contact with. [19]
Personal Hygiene and Health:
- Wash your hands regularly, especially after outdoor activities or contact with wildlife, farm animals, or pets. This helps reduce exposure and prevent the spreading of pathogens. [21]
- Maintain a healthy lifestyle by staying active, eating nutritious foods, staying hydrated, getting enough rest, and managing stress. This supports a strong immune system, which helps protect you from infections. [22]
Food Safety:
- Follow safe food handling and storage practices. Ensure animal products are cooked to the recommended temperature. Wash your hands thoroughly before and after handling raw or uncooked meat, seafood, and eggs.[23]
At Home and When You Travel:
- Increase ventilation in indoor spaces when possible. In crowded areas, consider wearing a mask and following other precautions if the risk of respiratory illness is high.
- Before traveling, research health risks for your destination, whether within Canada or abroad, and follow travel advisories and health guidelines.
We can work together to understand the risks and adapt our behaviours. We can also reduce our contribution to climate change. By understanding how climate change affects infectious diseases, and taking actions that will help prevent the spread of them, we can create a healthier environment for ourselves and our communities.
References:
- Mayo Clinic. Infectious diseases - Symptoms & causes. https://www.mayoclinic.org/diseases-conditions/infectious-diseases/symptoms-causes/syc-20351173
- Mora, C., McKenzie, T., Gaw, I.M. et al. Over half of known human pathogenic diseases can be aggravated by climate change. Nat. Clim. Chang. 12, 869–875 (2022). https://doi.org/10.1038/s41558-022-01426-1
- Vector Disease Control International (VDCI). Could Climate Change be Causing More Mosquitos? https://www.vdci.net/blog/could-climate-change-be-causing-more-mosquitoes/
- BCCDC. Zoonotic Diseases. https://www.bccdc.ca/health-info/disease-types/zoonotic-diseases
- Government of Canada. Current and future burden from Lyme disease in Québec as a result of climate change. https://www.canada.ca/en/public-health/services/reports-publications/canada-communicable-disease-report-ccdr/monthly-issue/2023-49/issue-10-october-2023/current-future-burden-lyme-disease-quebec-result-climate-change.html
- Khan, Ogden, Fazil, Gachon, Dueymes, Greer, and Ng. 2020. Current and Projected Distributions of Aedes Aegypti and Ae. Albopictus in Canada and the U.S. Environmental Health Perspectives 128. https://doi.org/10.1289/EHP5899
- Government of Canada. Increased risk of microbial foodborne diseases with climate change. https://www.canada.ca/en/public-health/services/reports-publications/canada-communicable-disease-report-ccdr/monthly-issue/2019-45/issue-4-april-4-2019/article-5-microbial-foodborne-diseases-climate-change.html
- Awad, D.A., Masoud, H.A. & Hamad, A. Climate changes and food-borne pathogens: the impact on human health and mitigation strategy. Climatic Change 177, 92 (2024). https://doi.org/10.1007/s10584-024-03748-9
- Herod, A., Goodridge, L., & Rohde, J. (2019). Recalls of foods due to microbial contamination classified by the Canadian Food Inspection Agency, 2000 to 2017. Journal of Food Protection, 82(11), 1901–1908. https://doi.org/10.4315/0362-028X.JFP-19-235
- Harper, S. L., Schnitter, R., Fazil, A., Fleury, M., Ford, J., King, N., Lesnikowski, A., McGregor, D., Paterson, J., Smith, B., & Neufeld, H. T. (2021). Food Safety and Security. In P. Berry & R. Schnitter (Eds.), Health of Canadians in a Changing Climate: Advancing our Knowledge for Action. Ottawa, ON: Government of Canada.
- Levy K, Woster AP, Goldstein RS,Carlton EJ. Untangling the Impacts of Climate Change on Waterborne Diseases: a Systematic Review of Relationships between Diarrheal Diseases and Temperature, Rainfall, Flooding, and Drought. Environmental science & technology. 2016:50:4905–22. Doi: 10.1021/acs.est.5b06186
- HealthLinkBC. Cyanobacteria blooms (blue-green algae). https://www.healthlinkbc.ca/healthlinkbc-files/cyanobacteria-blooms-blue-green-algae
- Mackenzie JS, Jeggo M. The One Health Approach-Why Is It So Important? Trop Med Infect Dis. 2019 May 31;4(2):88. doi: 10.3390/tropicalmed4020088. PMID: 31159338; PMCID: PMC6630404.
- University of Alaska Fairbanks. Center for One Health Research. https://www.uaf.edu/onehealth/
- Planetary Health Alliance. What is Public Health? https://planetaryhealthalliance.org/what-is-planetary-health/
- Government of Canada. Enjoy the outdoors, without a tick. https://www.canada.ca/en/public-health/services/publications/diseases-conditions/lyme-pamphlet.html
- Government of Canada. Mosquitos. https://www.canada.ca/en/health-canada/services/pest-control-tips/mosquitoes.html
- Government of Canada. Guidelines for Canadian recreational water quality: Summary document. https://www.canada.ca/en/health-canada/services/publications/healthy-living/guidelines-canadian-recreational-water-quality-summary-document.html
- CBC News. Why climate change might make you think twice about eating raw oysters this summer. https://www.cbc.ca/news/health/raw-oysters-vibrio-1.6862183
- Government of Canada. Creating a Healthier Canada: Making Prevention a Priority. https://www.canada.ca/en/public-health/services/health-promotion/healthy-living/creating-a-healthier-canada-making-prevention-a-priority.html
- Government of Canada. Food Safety Handling Tips. https://www.canada.ca/en/health-canada/services/food-nutrition/food-safety/safe-food-handling-tips.html
- Government of Canada. Respiratory infectious diseases: Reduce your risk. https://www.canada.ca/en/public-health/services/diseases/respiratory-infectious-diseases-reduce-spread-personal-protective-measures.html









.png)


