
Across Canada, the changing climate is affecting the health of people. [1] Prolonged periods of heat, wildfires and poor air quality, and infectious diseases are impacting our mental health, physical health, and the health of communities. We are realizing more and more that climate change is a health issue, as much as it is an environmental and social issue.
Good health and well-being are universal human rights. When everyone can attain their full potential for health and well-being it is called health equity.[2] In Canada and across the globe, governments and organizations have been working hard to increase health equity. A key group working towards this goal is health care professionals who work closely with community members.
Brigitte DeCosse is a community health nurse in Winnipeg, Manitoba, and a member of the Canadian Association of Nurses for the Environment. She explains that, “at the heart of community health nursing, instead of just caring for people at the individual and family level, we are also looking at the community as a whole.” DeCosse is a strong advocate for making changes to increase health equity, “we want to understand our communities, what inequities they are experiencing, and how to address them.” She acknowledges that climate change is making this more challenging.
“We can see that climate change is affecting all of our health… the health inequities that already exist will likely be amplified.” DeCosse points out how the biggest impacts will be felt by those most vulnerable in our society, but there are also opportunities. DeCosse emphasizes that “the way forward is as a community, as a society moving forward together helping each other”. If done in an inclusive manner, the actions that we take to address climate change can also work to improve health equity. “That’s how we will get the best results.”
Why does climate change impact the health of some people more than others?
There are individual characteristics and factors that can make climate change more impactful on one person’s health than another. During heatwaves for example, factors such as age, pre-existing health conditions, and access to air-conditioning can all play a role in how your health is affected.
“When we prepare for climate change, we need to take into account who is going to be affected the most. - Briggitte DeCosse”
This was the case during the heat dome in British Columbia in 2021, when a large pocket of heat sat over the west coast at the end of June. The heat dome lasted for 6 days. Temperatures reached into the high 30s, with little reprieve overnight. Over 600 deaths were attributed to the heatwave, becoming the deadliest weather-related disaster in Canadian history. [3]
According to the report to the Chief Coroner of British Columbia, the majority of those who passed away fell into one or more of the following categories: were older adults, had one or more chronic disease, and/or lived in housing with little to no ventilation. [4] The report highlighted how people experiencing those factors were over-represented, compared to the general population. Other factors, such as limited access to green spaces that can otherwise help keep temperatures cool, were also linked to increased health concerns. Many social and environmental factors contributed towards the severity of the event. [4]
Watch: Heatwaves, Health, and The Airconditioning Dilemma
The 2021 heat dome killed more people than any other natural disaster in Canada. In a world struggling with more frequent heat waves, this film investigates the delicate balance between the life saving use of air conditioning to stay cool and the environmental risks associated with its overuse. Researchers focused on the impact of rising temperatures on heart health explore the challenge of keeping cool without succumbing to the dangers of overheating. This documentary prompts viewers to consider the broader implications of our reliance on air conditioning, and offers cool solutions in an increasingly warming world.
When investigating patterns and trends in the health of populations, public health practitioners like DeCosse will look at factors called Social Determinants of Health (SDOHs). These are the social and economic factors that influence our health, including individual characteristics, income and wealth, social and cultural systems, education, health and healthcare access, and where we work and live. Differences in these factors are largely responsible for health inequities between populations.[5]
As we saw with the heat dome in western Canada, these differences in factors can contribute to how someone experiences a major event. When it comes to climate change and climate hazards, these differences can make some more vulnerable than others. That is why DeCosse emphasizes that “when we prepare for climate change, we need to take into account who is going to be affected the most.” This ensures that nobody is left behind.
As we saw with the heat dome in western Canada, these differences in factors can contribute to how someone experiences a major event. When it comes to climate change and climate hazards, these differences can make some more vulnerable than others. That is why DeCosse emphasizes that “when we prepare for climate change, we need to take into account who is going to be affected the most.” This ensures that nobody is left behind.
Read More: Examples of Social Determinants of Health
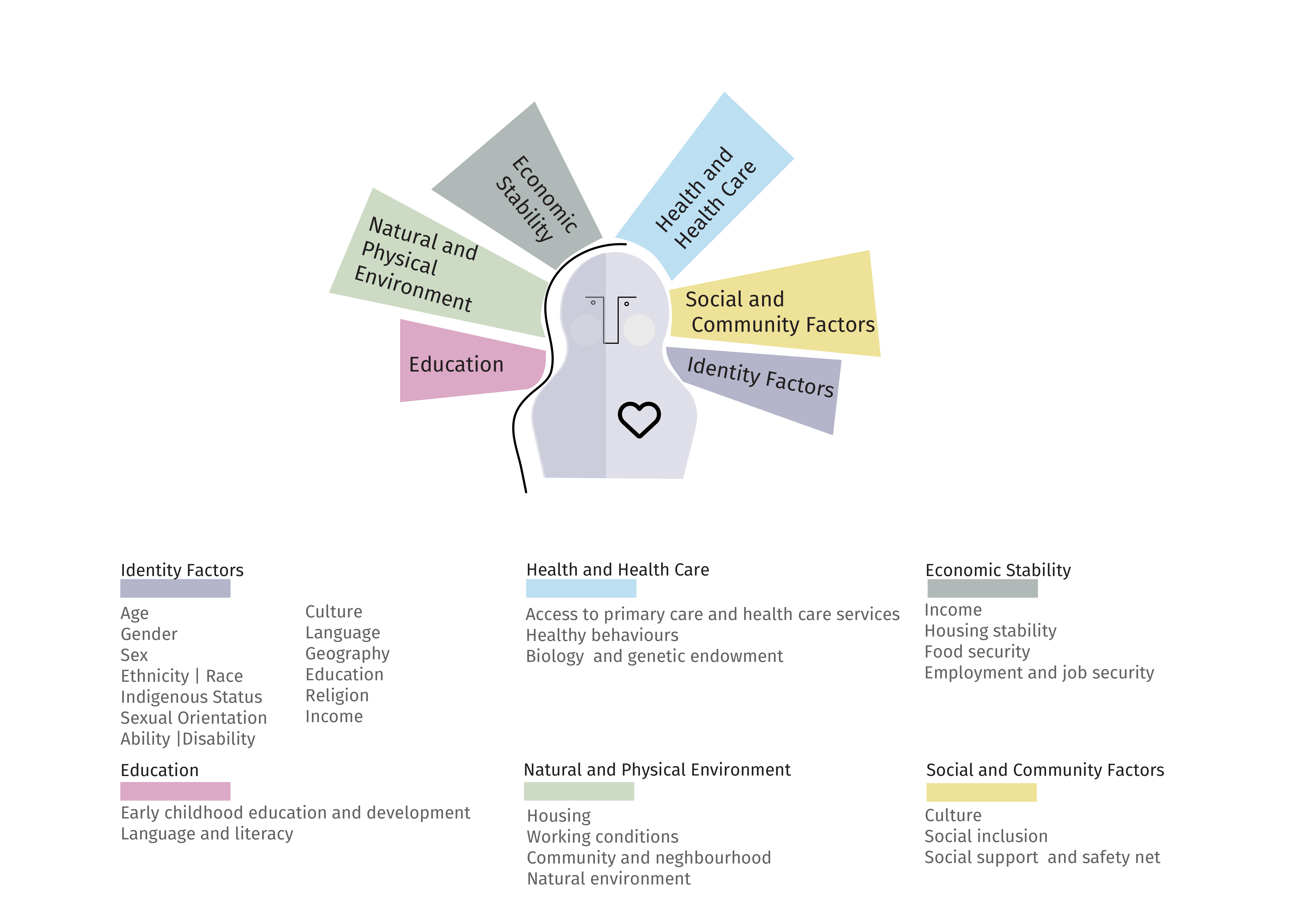
Social determinants of health can be thought of in several overarching categories such as education, natural and physical environment, economic stability, health and health care, social and community factors, and identity factors. These determinants can influence health positively or negatively. For instance having reliable access to adequate health care or stable housing contribute positively to our health, while lacking access to these factors can have negative impacts on health. The infographic below outlines some of these social determinants of health.
Read More: What is vulnerability, exposure, and resilience
Vulnerability, exposure, and resilience are concepts that are considered across many disciplines and fields of work. When used in conversation around climate change, they generally have these meanings:
Vulnerability: How susceptible a person is to an impact or climate hazard.
i.e. During wildfire season, how likely a person is to experience negative health impacts due to wildfire smoke. People who have pre-existing health conditions, like asthma, may be more vulnerable to the impacts of smoke.
Exposure: How likely a person is to encounter the climate hazard.
i.e. During wildfire season, how likely a person is to be in spaces with poor air quality. People who are required to work outside may have higher exposure than others.
Resilience: How well a person or community can overcome or bounce back from a climate related impact once it occurs.
i.e. How well a person can handle days with poor air quality. If a person is in good health, and/or has access to clean air spaces, they have higher resilience to days with poor air quality.
Vulnerability, exposure, and resilience can be hard to quantify, but they work hand in hand to create a picture of how much a person may experience the negative impacts of a climate hazard or impact.
Intersectionality
Talking about health and vulnerability can be complicated. The factors that influence them, like gender, race, culture, class, age, and sexuality, combine and interact to make everyone’s experiences different. “They set our perceptions, the values that we hold, and the way we approach the world,” says Dr. Amber Fletcher. Dr. Fletcher is a professor in the Department of Sociology and Social Studies at the University of Regina in Saskatchewan and the director of the Gender, Environment, and Social Inequity Research Lab at the University. Looking at social inequity issues is a core part of Dr. Fletcher's work. “My research is focused on talking to people and understanding how they experience the world, how they perceive challenges, and the social forces that shape their response to major phenomena like climate change”.
Dr. Fletcher emphasises the importance of considering intersectionality when addressing challenges like climate change. She explains that social systems and structures such as racism, patriarchy, capitalism, ableism, ageism, and colonialism exist at the same time, and “these different systems of power and privilege come together to create very different diverse experiences for different people.” These experiences are important to consider, as vulnerability to climate change is made worse by the marginalization caused by these systems and structures. [5]
“It’s nuanced,” Dr. Fletcher continues, “the kinds of inequity and oppression that are experienced are different between groups and individuals.” Understanding how people perceive, interact with, and experience the world is important “if we want to build policies that work effectively for all people, want interventions that facilitate equity, and don't reproduce a lot of the problems that we currently see.” Dr. Fletcher believes intersectional approaches to addressing climate change create more equitable outcomes, which improves health equity.
Watch: Cripping Climate Adaptation - Disability Justice
People with disabilities are the world's largest minority group and are disproportionately affected by climate change. As disability justice and climate issues collide, Cripping Climate Adaptation lays bare the often disastrous consequences of overlooking people with disabilities and illustrates the need to consider the unique needs of people with disabilities and include them in climate adaptation.
Set to a lively visual backdrop of dance, music, and activism, this documentary defines the incredible toolkit on adaptation from the disability community, one that adds depth, texture and creativity to get beyond traditional ways of how the environment is used. Let's not miss out on this tool kit of ways of seeing.
Bringing Equity into Climate Change Planning
Creating a more equitable future requires change. Decisions made at all levels of community and society need to better integrate diverse perspectives, especially those historically excluded from the conversation, who are the same people often experiencing these impacts the most. From Dr. Fletcher’s point of view, working together and including these perspectives is critical, “if we want our work to inform policy responses or adaptation planning, it has to be connected to what matters to people, to the values that people have and the concerns that people experience within communities.” And the first step in this process? “We have to talk to the people that are affected,” Dr. Fletcher states.
“Communities and groups, especially those already experiencing inequity, have so much knowledge about how the system works because they encounter it every single day.” Dr. Fletcher continues, “Recognizing their knowledge, their agency, the things they're already doing, and being able to amplify that ensures that it gets built into whatever responses and plans get developed for climate change.”
System change might seem daunting but starting with small actions can help move us in the right direction. To create a more equitable future, Decosse suggests we need to “start having more conversations about health inequities and the root causes of why we're seeing them”. She additionally suggests “working together instead of in silos” is also part of the solution.
This shift in thinking is already happening, and this makes DeCosse hopeful, “we are already starting to see this shift in consciousness, from a more individualistic way of living towards a more community driven way of living… The way forward is as a community and society moving forward together.”
References
- Berry, P., & Schnitter, R. (Eds.). (2022). Health of Canadians in a Changing Climate: Advancing our Knowledge for Action. Ottawa, ON: Government of Canada.
- World Health Organization. Health Equity. 2026. Retrieved from https://www.who.int/health-topics/health-equity
- Yoon, L., Richardson, G. R. A., & Gorman, M. (2024). Reflections on a century of extreme heat event‐related mortality reporting in Canada. GeoHealth, 8, e2023GH000895. https://doi.org/10. 1029/2023GH000895
- BC Coroners Service . (2022a). Extreme heat and human mortality: A review of heat‐related deaths in B.C. in summer 2021. Retrieved from www2.gov.bc.ca/assets/gov/birth-adoption-death-marriage-and-divorce/deaths/coroners-service/death-review-panel/extreme_heat_death_review_panel_report.pdf
- Canadian Public Health Association. What are social determinants of health? Retrieved from: https://www.cpha.ca/what-are-social-determinants-health
- IPCC, 2022: Summary for Policymakers [H.-O. Pörtner, D.C. Roberts, E.S. Poloczanska, K. Mintenbeck, M. Tignor, A. Alegría, M. Craig, S. Langsdorf, S. Löschke, V. Möller, A. Okem (eds.)]. In: Climate Change 2022: Impacts, Adaptation, and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change [H.-O. Pörtner, D.C. Roberts, M. Tignor, E.S. Poloczanska, K. Mintenbeck, A. Alegría, M. Craig, S. Langsdorf, S. Löschke, V. Möller, A. Okem, B. Rama (eds.)]. Cambridge University Press, Cambridge, UK and New York, NY, USA, pp. 3-33, doi:10.1017/9781009325844.001.









.png)


